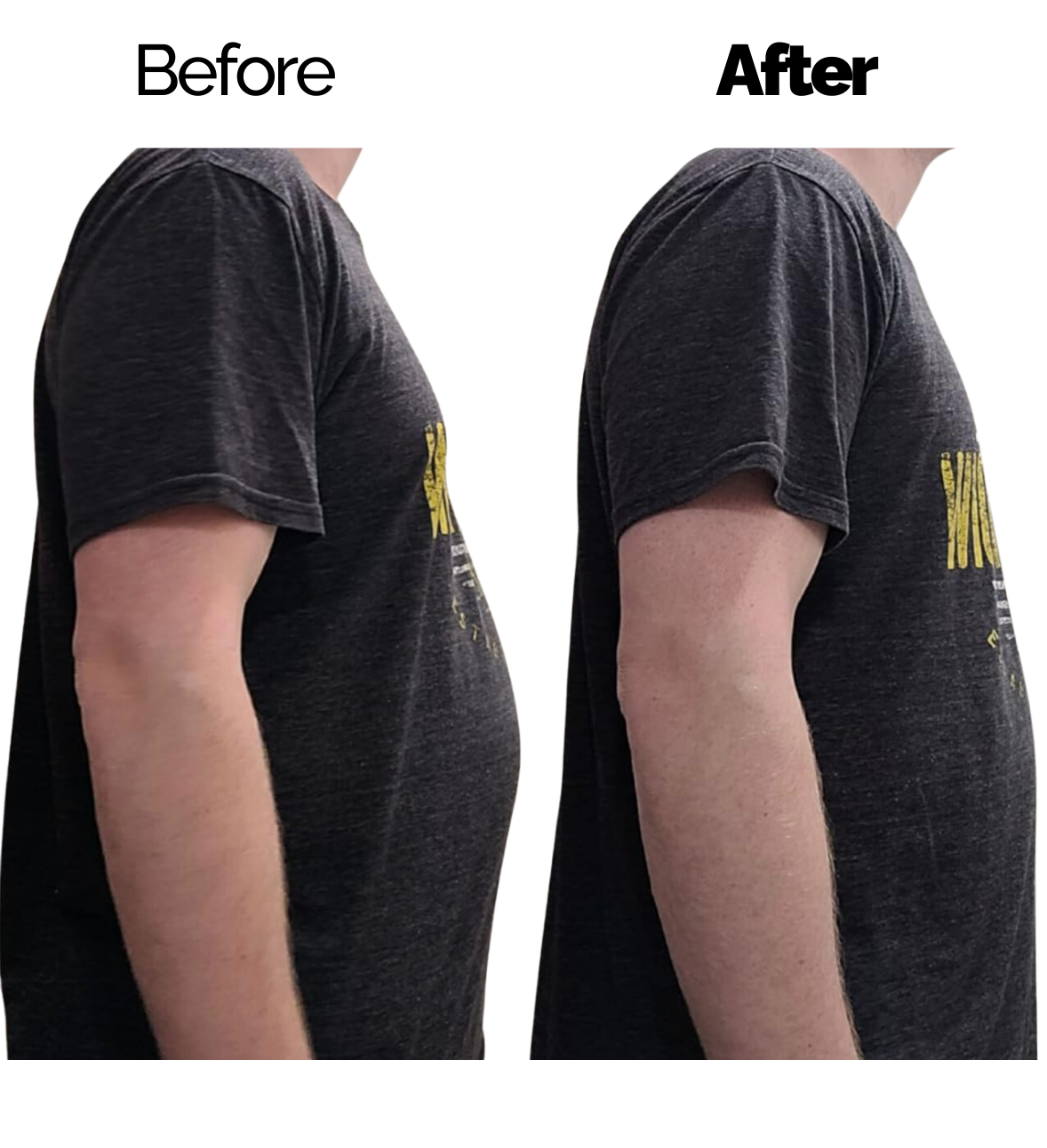
Gynecomastia causes male breast tissue to grow larger. This happens to babies, teens, and grown-ups. Hormone issues being overweight, or some medicines can cause it. Gynecomastia has an influence on how a man feels about himself and his life. This leads many men to think about surgery.
Why insurance often won't pay for gynecomastia surgery
Even though gynecomastia affects men's minds and bodies, getting insurance to pay for surgery is tough. Most insurance companies think gynecomastia surgery is to look better, not for health reasons. This view makes it hard for patients to get insurance to cover it. As a result, patients often face big costs.
Step 1: Documenting the medical necessity of gynecomastia surgery
To overcome obstacles to insurance coverage, you need to provide thorough proof of the medical necessity for gynecomastia surgery. This proof should contain medical records physical exam results, and any diagnostic tests that show the need for surgery. Also, it helps to include psychological assessments or therapy notes that show how gynecomastia affects the patient .
Step 2: Reviewing your insurance coverage and policy
Before you go ahead with gynecomastia surgery, you should check your insurance coverage and policy. Get to know the terms and conditions about coverage for cosmetic procedures pre-authorization needs, and any exclusions that relate to gynecomastia surgery. When you understand your policy, you can stand up for yourself better and make sure you meet all the needed criteria for insurance coverage.
Step 3: Collecting supporting documents for insurance claims
After you've got a good grasp of what your insurance covers, you need to collect all the paperwork to back up your insurance claims. This includes your medical files results from diagnostic tests letters from your doctors saying the surgery is needed, and any other important papers. It's key to put together a complete file that shows why gynecomastia surgery is necessary.
Step 4: Filing the insurance claim for gynecomastia surgery
Now that you've got all the backup paperwork ready, it's time to send in your insurance claim for gynecomastia surgery. Make sure you follow your insurance company's rules for submitting claims. Double-check that you've filled out all the required forms and included all the supporting documents. Be ready for possible delays, and don't forget to check in with your insurance company to make sure they're working on your claim.
Step 5: Dealing with insurance denials and appeals
Sometimes, insurance companies might say no to paying for gynecomastia surgery. If they turn you down, don't give up. You can often change their minds by appealing. Take a good look at the letter that says why they said no, and get any extra info or papers that could help your case. Team up with your doctors to make a strong appeal and do what your insurance company says you need to do.
Other ways to pay for gynecomastia surgery
When insurance doesn't cover gynecomastia surgery or denies your claim, you still have ways to pay for it. Some doctors let you spread out the cost with payment plans or other funding choices. Also certain companies give out medical loans just for health treatments. Look into these options and pick the one that works best for your wallet.
Choosing the right surgeon for gynecomastia surgery
When you're thinking about gynecomastia surgery, picking the right surgeon is key. Look for a plastic surgeon certified by the board who knows male breast reduction inside and out. Set up meetings with several surgeons to talk about what you want, ask them about their background, and check out their before and after pictures. Take your time to find a surgeon who gets what you need, puts you at ease, and has a history of good results.
Conclusion: Breaking down barriers to gynecomastia surgery coverage
Getting your insurance to cover gynecomastia surgery isn't easy, but it's doable. To boost your chances make sure to document why you need the surgery, know your insurance policy inside out, and file a detailed claim. If they say no, don't give up – look into other ways to pay for it. And when you're ready, pick a top-notch surgeon who knows their stuff when it comes to gynecomastia. If you stick with it and get the right help, you can overcome the hurdles to getting coverage for your surgery. This can help you feel better about yourself and improve your life overall.
If gynecomastia is giving you trouble and you want your insurance to cover the surgery, keep trying. Follow the steps in this guide and talk to a board-certified plastic surgeon who knows how to do male breast reduction. Keep in mind, you can overcome obstacles, and you have the right to live without the physical and emotional weight of gynecomastia.